Eight years of conflict and crisis in north-eastern Nigeria have left two-thirds of health facilities completely or partially destroyed and millions of people without access to healthcare. In August last year, when health teams managed to reach previously inaccessible areas, they found a critical situation. Functioning health facilities were overburdened and more than 40% of Internally Displaced Persons (IDP) camps had no access to basic healthcare services. Childhood vaccination rates had dropped dramatically, leaving children at risk of life-threatening diseases such as polio, whooping cough, pneumonia and measles, and the rate of severe acute malnutrition was estimated at 14%.
In view of these findings, WHO scaled up its support to address people’s health needs and to implement innovative interventions aimed at reducing health risks. Despite continued insecurity, wherever WHO and partners are able to reach those in need, their goal remains the same: to reduce the risk of disease outbreaks and bring life-saving health services to those who need them.
WHO Mobile health teams delivering healthcare in remote areas with no access for years

In north-eastern Nigeria, access is becoming more challenging due to insecurity, difficult terrain and poor road networks. The conflict has also led to an exodus of skilled health-care workers, leaving many people without basic healthcare.

The 113 WHO-supported mobile health teams across Borno, Yobe and Adamawa states are trying to fill this gap. The teams have seen more than 400 000 clients, treated some 83 000 people across 25 areas in Borno state since August 2016.
Community Resource Persons (CORPS): providing integrated community case management of childhood diseases

In line with the Integrated Maternal, Newborn, Child Health strategy, WHO trained and engaged 680 Community Resource Persons to provide integrated community case management of childhood diseases.
These community-based volunteers are trained by WHO to assess, classify and treat childhood illnesses. They have reached more than 50 000 children in 680 communities with various healthcare services ranging from treatment of minor illnesses to health promotion across Borno, Adamawa and Yobe states.
By training community members, WHO and partners are bringing health to people who might have previously had to travel long distances in unsafe environments.
WHO supports 400 000 severe acute malnourished children in the north-eastern Nigeria
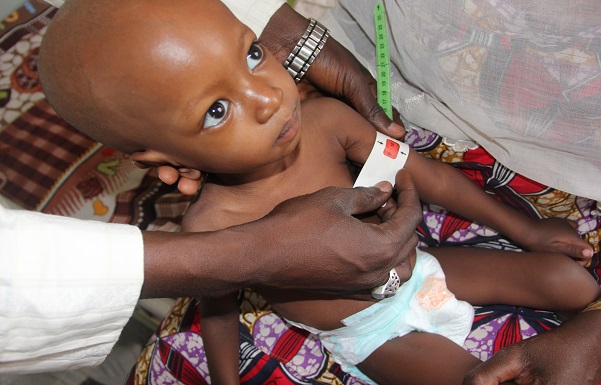
An estimated 400 000 children in north-eastern Nigeria are currently suffering from severe acute malnutrition. Without proper treatment, one in five of those children – around 75 000 – could die.
So far 50 WHO severe acute malnutrition (SAM) kits have been provided to 16 health facilities in Borno and Yobe states for the stabilization centers. The kits contain medicines including antibiotics, antimalarial, treatment for diarrhoea, diagnostic kits for diseases like malaria, and supplies including thermometers, gloves and syringes. One SAM kit is designed for the management of medical complications from severe malnutrition for 50 children for around 3 months. Over 1,500 children that have severe acute malnutrition with medical complications been treated at the centres and more than 180 000 children have been screened for acute malnutrition.
The volunteers have reached more than 87 000 mothers and caregivers educating them on infant and young child feeding, and 8,413 children 6-23 months reached with micro-nutrient powder to prevent and control micro-nutrient deficiencies.
Reducing malaria morbidity and mortality among children under-5
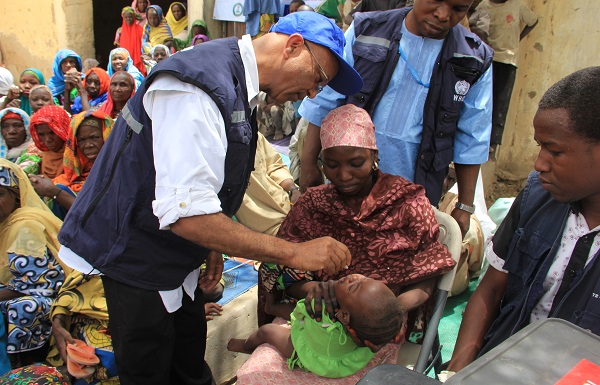
In Borno state, WHO estimates more than half of recorded deaths are currently due to malaria, more than all other causes of death combined, including cholera, measles and hepatitis E. A highly vulnerable population, consisting largely of children (58.8%), is at risk. However, malaria is preventable and curable.
In collaboration with health authorities, WHO launched 4 rounds of seasonal malaria chemoprevention campaign to reach children under-five that are especially vulnerable to malaria. The first round reached in July 2017 more than 880 000 in Borno state.
Malaria is a life-threatening disease caused by parasites that are transmitted to people through the bites of infected mosquitoes. More than 90% of malaria deaths occur in Africa.
Leading and coordinating 22 health sector partners to deliver targeted healthcare services to 5.9mliion people in northeast Nigeria

WHO has developed preparedness and response plans to respond to cholera, cerebro-spinal meningitis, and hepatitis E. The plans helped guide the prepositioning of diarrheal disease kits in identified “high risk/hot spots”, reproductive health kits and severe acute malnutrition kits to more than 127 health facilities in priority Local Government Areas across Borno state.
Over 3 million people were reached with health services in the first half of this year by the health sector.
Surveillance: Catching up with disease outbreaks at outbreak thresholds

Within two weeks of scaling up its emergency response in late August 2016, WHO rolled out its Early Warning Alert Response System (EWARS) in 56 health facilities across Borno state. By mid-October, as access to some hard-to-reach areas improved, the number of disease detection sites increased to 239. Now 239 sites in Borno state are using the system, covering around 85% of internally displaced persons living in Borno state or 1.3 million people.
WHO’s EWARS supports disease surveillance, alert and response even in the most difficult operating environments. EWARS helps alert health authorities to disease outbreaks early on to help contain them in emergencies.
Strengthening humanitarian support through Health logistics

To strengthen the preparedness and response capacity for viral hemorrhagic fever (VHF), WHO constructed VHF treatment centre and trained 42 health care providers (doctors, nurses, environmental health workers, security hospital cleaners) that will provide services. WHO and partners responded to 6 cases of VHF (Lassa) that were detected earlier this year.
WHO has rehabilitated a public health emergency operations centre to provide an operational space, equipment and procedures necessary for effective coordination and timely decision-making required in a public health emergency.
Challenges

Humanitarian work in the affected areas is still extremely challenging. Resources and capacities to meet the enormous health service gaps are grossly inadequate. Insecurity is a major constraint, with a number of recent attacks on humanitarian staff. To further exacerbate the situation, the annual wet season has peaked and there are forecasts of major floods that often bring cholera and other water-borne diseases. Access to many locations still requires a helicopter and military escorts.
Nonetheless, in collaboration with the government and partners, WHO is taking bold steps to tackle the health challenges in the region. WHO has already set up an emergency response team and deployed both national and international emergency staff to coordinate, plan, respond, and monitor WHO emergency operations in north-eastern Nigeria.
